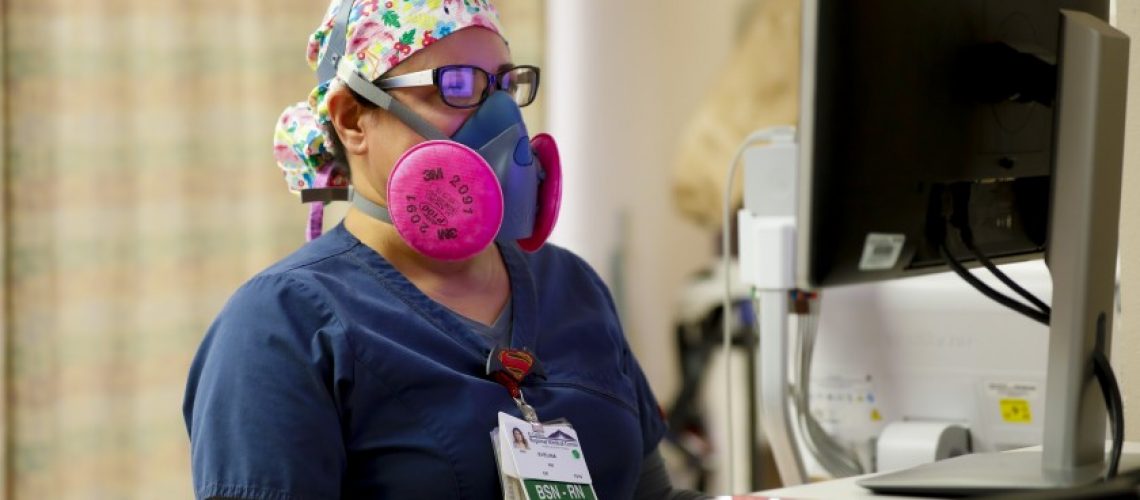
The emergency department is often the place one sees the carnage at the other end of failed policies. We see that with COVID-19, traffic collisions and drugs.
Public health means caring about the overall health of a population. The Centers for Disease Control definition of public health is “the science of protecting and improving the health of people and their communities.” Public health policies calculate and balance individual behavior and preference, economics, and the benefit for the community at large.
Sometimes good public health policies come at the cost of an individual’s convenience. A classic example of such a health policy is wearing masks to prevent the spread of COVID-19. Who likes wearing a mask? I don’t. It hurts my face.
Another example of a successful public health measure is seat belts. My first car was an orange 1972 Volkswagen Beetle that came with a useless lap belt that was way too big for me. I recall the debate by people who did not like the restrictions of seat belts and claimed that mandatory seat belts violated their freedom and constitutional rights. According to the National Highway Traffic Safety Administration, in 1990, only 50% of Americans wore seat belts. Now seat belts are a habit most people don’t even think about. Today, 90% of people buckle up. This public health policy saved 15,000 lives in 2016 and would have saved 2,500 more if everyone complied.
Today motorcyclists still complain that helmets cause headaches, tunnel vision and that “it’s nobody’s business if I want to feel the wind in my hair.” In emergency departments and trauma centers, motorcycles accidents had an association with brain death injuries resulting in organ donation. Helmet laws changed that. In 2016, helmets saved 1,859 motorcyclists’ lives and 802 more lives could have been saved if all motorcyclists had worn helmets. I argue that it has proven to be a worthwhile inconvenience.
American innovation, regulation and focus on traffic safety continue to save lives. Traffic fatalities peaked in 1937 with 30.8 deaths per 100,000 population. The most recent data from 2018 is 11.17 deaths per 100,000. This improvement of over 60% occurred despite a marked increase in total miles driven and number of cars on the road. Improved traffic safety was no accident. This remains a major focus on multiple levels. Individuals made sacrifices by wearing seat belts and helmets. The automotive industry introduced advanced engineering such as airbags, electronic stability, backup cameras and blind spot detection. Government worked on improved roads and traffic laws.
I am jealous of the efforts for car safety. We desperately need the same multidisciplinary approach for drugs and addiction. Sadly, wise public health decisions are getting pushed aside for economic benefit and the call for individual freedom. For example, electronic cigarettes hit the market without appropriate public health consideration. The industry used an untested health claim that vaping helps tobacco cessation to promote its products. However, epidemiologic studies show that for every one adult who quits cigarettes using e-cigarettes, 80 adolescents who never smoked will eventually become daily smokers through e-cigarette use.
Similarly, marijuana legalization, both medically and recreationally, is driven by economics and individual freedoms, rather than public health consequences. Public health consideration would account for the total associated increase in drug use and emergency visits, and the various medical complications. I do not wish to judge or shame people who choose to use marijuana, but I strongly believe that the public has the right to informed decisions. People who smoke cigarettes understand the risks of addiction, cancer, emphysema and heart disease. People who use marijuana are sold on the multiple benefits without education on drug interactions with prescription medications, high potency psychosis and suicide, testicular cancer, and pulmonary or heart risk.
San Diego leads the county with one of the best trauma systems in the world. Saving a trauma patient can require a blood transfusion, but for the bleeding to stop, the hole needs to be plugged.
Addiction prevention means preventing any addictive substance use while the brain is growing. Brain development continues until age 25 or 27. The chances of addiction for someone under this age is four to seven times higher than for older people. Policies that promote increased marijuana and drug use, along with the normalization of drugs, sacrifice our youth and therefore our future for the benefit of the individual. We need strong public health consideration when it comes to drug policy.
Lev is an emergency/addiction physician at Scripps Mercy Hospital and former chief medical officer at the White House Office of National Drug Control Policy. She lives in Poway.
Originally published at: https://www.sandiegouniontribune.com/opinion/commentary/story/2020-12-04/public-health-policy